A LONG JOURNEY
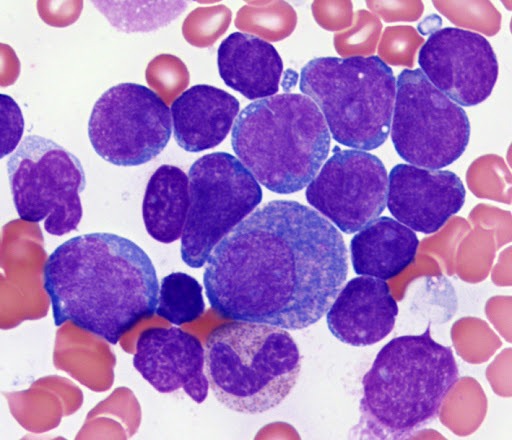
Acute lymphoblastic leukaemia (or A.L.L.) is a type of blood cancer that involves the bone marrow. It affects one particular type of white blood cell – called lymphoblasts. They multiply uncontrollably, first in one spot and then in nearby tissues. This form of leukaemia is considered rare but is still the most common leukaemia in children, although it affects all age groups. It affects children more than adults, and men more frequently than women. It most likely occurs between 0 and 5 years of age.
80%
A.L.L. makes up 80% of
all childhood leukaemias
(below 15 years)
300
More than 300 adults and
children are diagnosed with
A.L.L. each year in Australia

It is considered particularly aggressive, so is treated as an emergency once diagnosed. In the past ten years, medical advances and the introduction of new treatments have allowed remarkable progress in cure rates, mainly in children, who withstand chemotherapy better than adults.
Bone marrow, the producer of blood cells
Leukaemia affects the bone marrow, the place where all blood cells are produced. These cells include red blood cells (responsible for transporting oxygen), white blood cells (that defend the body against infection), and platelets (which aid in clotting). In Acute lymphoblastic leukaemia, lymphoblasts multiply in an uncontrolled way, instead of growing into mature cells and moving into the blood. They then interfere with the normal production of blood cells. They may also reach other organs, such as the lymph nodes, liver and spleen.
Risk Factors
Acute lymphoblastic leukaemia has no known cause or triggering factors. It is not contagious or hereditary. Some risk factors have been identified:
- Exposure to ionizing radiation: accidental, therapeutic (radiation therapy), or occupational
- History of chemotherapy, administered during a prior cancer
- The presence of certain genomic anomalies, including Down syndrome
- Pre-existing blood conditions
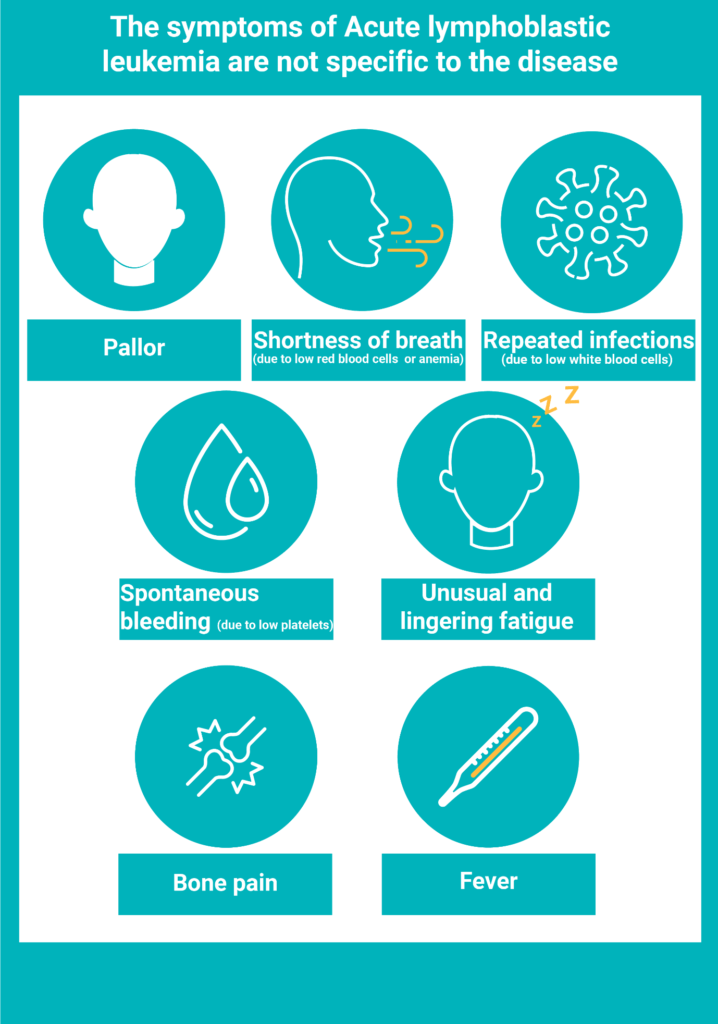
Symptoms
Treatment
Acute lymphoblastic leukaemia must be managed quickly. As the bone marrow is invaded by abnormal cells, severe infection (as the consequence of a reduction in normal white blood cells) or bleeding (as a result of reduced platelet production) can occur. The haematologist decides which treatment is most suitable for each patient, most likely lasting 2-3 years, given in several phases:
Induction treatment, with hospitalisation for at least a month. The purpose is to eliminate cancerous cells, which will enable a regeneration of normal blood cells.
Consolidation treatment, sometimes a bone marrow transplant is suggested. This transplant comes from a compatible donor (family or donor registry), but can also be obtained from placental blood, called cord blood.
Maintenance treatment is administered for two years to prevent relapses. The patient sees the doctor as an outpatient during this time.
Reinduction treatment A new chemotherapy is given if patients do relapse, again followed by consolidation and maintenance treatment.
At Servier
Servier currently invests a large part of its budget in oncology research and development, with the goal of improving management of patients with blood cancers. Possibilities being followed by Servier’s R&D teams are: to better understand the pathways that lead to the development of the disease or resistance to standard treatments, searching for new ways to treat the disease and researching which treatments may be the most appropriate for each patient.
Key points
- Acute lymphoblastic leukemia is a rare disease that affects children more than adults.
- It doesn’t present specific symptoms and its cause is currently unknown.
- During the past few years the management of this disease has made considerable progress leading to high cure rates, particularly in children.
References:
- American Cancer Society – July 2019. SANTÉ PUBLIQUE France /INCaParkin DM et al. eds. International incidence of childhood cancer, Vol. II. Lyon, International
- Agency for Research on Cancer – WHO Fact Sheet 2009 Hunger SP, Mullighan CG. Acute Lymphoblastic Leukemia in Children. NEJM 2015;373(16):1541-1552.Sant M et al. Blood. 2010;116(19):3724-3734. Coebergh JWW et al. Eur J Cancer. 2006;42(13):2019-2036.